My ectopic pregnancy story…
From the second I found out I was pregnant, I knew there was something wrong.
Actually, let me rephrase that: part of the problem was that there WAS no “second” when I found out I was pregnant.
Instead, it took four days.
The first test was negative.
The next one – a day later – was faulty. Seriously, what are the odds?
The one after that showed a very faint positive… and the one after that was negative.
Thinking that maybe the batch of cheap pregnancy tests I’d bulk-bought from eBay were faulty, or had been kept too long in the wrong temperature or something, I sent Terry out to buy me a proper, brand-name test.
He came back with a brand I didn’t recognise… and it was ALSO faulty.
*HEADDESK*
Out he went again, this time returning with, not one, but TWO different test kits, from two different brands. In absolute despair, I took both of them simultaneously, by using the very dignified method of peeing into a cardboard cup, and then dunking both tests together, so they were both taken under exactly the same circumstances.
One was positive (but only just), the other was negative.
I. Was. Beside. Myself.
A few hours later, I got a slightly stronger positive, and then, not one hour later, I started spotting.
GOD.
I was in absolute despair by this stage. I knew you can’t get a false positive on a home pregnancy test (or that it’s very rare, anyway), so I was pretty sure I was pregnant now, but… well, if there’s such a thing as a little bit pregnant, I was it. It seemed very obvious to me that this very fragile little pregnancy wasn’t going to last, so, over the next few days I tried to steel myself for what I assumed was the inevitable miscarriage, and NOT the ectopic pregnancy story I’d always feared would happen to me.
But the miscarriage didn’t come.
The spotting didn’t stop either, though, and I was having absolutely no pregnancy symptoms, so, on day five or so (The timeline’s all a bit of a blur now, I’m afraid) we called up the early pregnancy unit – who I was, unfortunately for me, very familiar with, following my miscarriage, just two months earlier.
The nurse in charge of that unit is called Jill, and she is one of the nicest people I’ve ever met. This was some small comfort to me as I sat in a hospital room, just a few hours later, having my blood taken for the very first time in my life.
Unfortunately for me, it wasn’t to be the last time, either. Far from it, in fact.
That initial blood test, you see, doesn’t really do much more than confirm you are, in fact, pregnant, by measuring the level of the pregnancy hormone, HCG, in your blood. What’s important here, though, isn’t the initial number – it’s what that number does over the next 48 hours or so. In a normal, healthy pregnancy, your HCG level should more-or-less double in that period of time: so I’d have my blood taken for the initial reading, Jill told me, and then I’d have to come back two days later, to have the HCG level measured again. Awesome!

My ectopic pregnancy story: diagnosis
Although we’d been told the initial number wasn’t really important, we still had a pretty tense wait for the phone call confirming it: and, when it came, the news wasn’t great. As I’d expected, the test confirmed I was pregnant… but my HCG had measured at just 192 – which was really quite low for my stage of pregnancy. Jill reminded us that this number wasn’t the important one, and even said she’d known women with very low initial HCG, who’d still gone on to have totally normal pregnancies – but she also admitted that the number wasn’t encouraging, and when we ended the call, we both had a bit of a cry, knowing this was likely to be yet another miscarriage, and that it was really just a matter of time before it happened.
I was absolutely devastated, as you can probably imagine: I still wasn’t over my first miscarriage (I actually don’t think you EVER really get over something like that… ), and now I was faced with going through the same thing again, which was just… yeah. Oddly, though, the spotting seemed to reduce, and no matter how hard I tried, I just couldn’t quite bring myself to stop hoping that maybe everything could still work out: maybe the next blood test would show the HCG doubling after all, and everything would be OK?
Yeah, it wasn’t.
The next book test showed the HCG increasing to 221 – which was more than we’d expected, granted (We still thought it was “just” a miscarriage at this point, so we’d expected the levels to DROP…), but not nearly enough to indicate a healthy pregnancy.
“I’m really sorry,” said Jill, when she called with the news, “But we don’t think the pregnancy is viable. We think you’ll probably miscarry within the next couple of days.”
So we waited for that to happen: and if you’ve ever had to wait for a pregnancy you know isn’t viable to end, you’ll know EXACTLY how heart-breakingly awful those next two days were.
The miscarriage didn’t come, though: and here’s the thing that amazes me when I look back on all of this:
It STILL didn’t occur to me that the pregnancy might be ectopic.
That probably sounds a bit odd to most of you. I mean, why WOULD I think that, right? Ectopic pregnancies aren’t uncommon, but they’re spoken about even less than miscarriage is: when mine was finally confirmed, I had to explain to quite a few of my friends what it actually WAS. I’d always known about ectopic pregnancy, though, because my mum had had her own ectopic pregnancy story to tell a couple of years after I was born. I’d grown up hearing the stories about it – and I’d also grown up absolutely convinced that, if I were to ever get pregnant, the same thing would happen to me. In fact, I was SO scared of that happening that, the first time I got pregnant, I actually paid for a private scan at 6 weeks, just to rule out the possibility of it being ectopic.
This time around, however, it hadn’t even occurred to me – probably because, by that stage, I already had one recent miscarriage behind me, and now THAT had become my biggest fear. Also, what were the odds that I’d end up getting the same pregnancy complication as my mum? Or of the one thing I feared more than anything else actually happening?
Er, pretty high, as it turned out.
When the results of my third blood test came back, it was the same thing again: the numbers had risen, but not enough to mean the pregnancy was viable. And now, for the first time, the word “ectopic” was being mentioned.
It was late on a Friday afternoon when we got the call. The doctor didn’t THINK the pregnancy was ectopic, Jill assured me…. but he wanted me to come in on Monday for an ultrasound scan just to rule it out.
Jill was doing her best to be reassuring – but I completely lost it. So much so, in fact, that Terry ended up having to get me an emergency appointment with my GP, who prescribed Valium to try and calm me down.
It didn’t work. I was SO terrified that I was going to need surgery – or that, if the pregnancy WAS ectopic, that it would rupture the tube while I was waiting for the scan – and I just couldn’t stand the thought of having to live with that fear all weekend. I begged Jill to try and get me an earlier scan, but the ultrasound department at our local hospital was already closed for the weekend, so Terry called the Edinburgh Royal Infirmary, which carries out scans all weekend, to try to get me an appointment there.
My ectopic pregnancy story: the scan
They refused to give me one – right up until the point where the nurse on the phone heard me sobbing in the background, and grudgingly agreed to fit me in the next morning, while making it clear that it was a huge imposition, as she’d looked at my chart, and thought it was unlikely the pregnancy was ectopic. (I got just a tiny bit of pleasure out of the contrite look on that nurse’s face when she was proved wrong the next day…)
I just KNEW it was, though. There was absolutely no doubt in my mind that the scan would confirm my worst fears – so much so that I actually brought a packed hospital bag with me the next day as we drove to the hospital.
I don’t think I’ll ever forget that waiting room, with it’s little Christmas tree, its Adele songs playing on repeat, or its depressing posters detailing all of the different things that could go wrong with a pregnancy. We seemed to sit it for an absolute eternity, but finally Terry and I were shown into a scan room, where a very serious looking sonographer, and a stern faced nurse were waiting.
The scan was an internal one, and seemed to last forever. Eventually, though, the sonographer turned away from the screen and looked me in the eye.
“I can’t find any trace of a pregnancy in the uterus,” she began, getting straight to the point. “But then again, I wouldn’t really expect to, given how early it is.”
My heart leapt. Maybe it wasn’t ectopic after all?
Er, no, Amber. Sorry.
“I can, however, see a small shadow in the right fallopian tube, right next to the ovary,” the sonographer continued. “I can’t be 100% sure it’s a pregnancy,” she said. “It could just be the side of the ovary.”
My heart leapt again. But not for long.
“Amber,” the sonographer said, looking even more serious than before, “I’m not telling you that you have an ectopic pregnancy: it’s too soon to really be sure. But given the blood results, I think they’ll want to treat it as if it is one, so I’ll go and get the doctor, and she can talk to you about what happens next.”
And then I burst into tears, obviously.
I can still vividly remember the next few minutes, and how utterly surreal they were. I just couldn’t believe my worst fear had come true: that I ACTUALLY had an ectopic pregnancy – the very thing I’d spent most of my life worrying about – and that now I might need surgery. I was still shaking with fear as we were shown into the office next door, and I kept on shaking until the doctor arrived – looking implausibly young and fresh faced.
Like the sonographer, she got straight to the point.
Treatment options for ectopic pregnancy
“We’re 99% sure your pregnancy is ectopic,” were her opening words to me. “So we need to act really quickly to make sure the fallopian tube doesn’t rupture.”
By this point, I was actually too freaked out even to cry. All I could think about was the fact that I might need to have surgery (I have an extreme phobia of general anaesthetic, and of hospitals…), and the need to avoid that at all costs, so I was relieved when the doctor told me I had three options.
The first was to do nothing, and just hope the pregnancy ended on its own. This option wasn’t, however, one the doctor was willing to consider, as my HCG was still increasing, meaning there was a real risk of the fallopian tube rupturing.
The second option was to treat it with methotrexate – a drug normally used in chemotherapy, but which would basically stop the pregnancy growing, and dissolve it in the tube.
And the third option? Was surgery.
“I’d literally rather die,” I told the doctor, aware of how ridiculous I sounded, but already past caring.
“Well, we won’t go for that option, then,” she said kindly. “Or not as long as option 2 works, anyway…”
And so it was that I found myself leaving the hospital with a pile of paperwork on ectopic pregnancy, and strict instructions not to do anything too energetic – even housework was forbidden, as it could cause the tube to rupture – and to come back the next morning to have the methotrexate injection. (In my ass, naturally. I get all the luck…)
I was just BEYOND devastated. I’d been prepared to be told the pregnancy had ended – I already knew it wasn’t viable – but absolutely nothing can prepare you for being told the pregnancy HASN’T ended….but that, unless it does, it’ll kill you.
I didn’t get much sleep the next night, needless to say – or any night after that, for that matter.
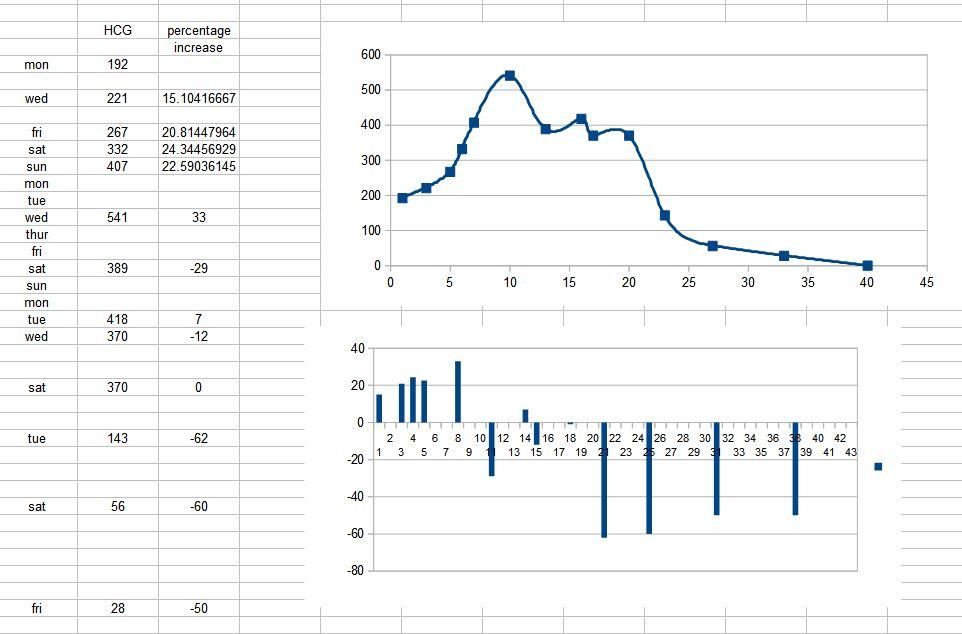
MY ECTOPIC PREGNANCY STORY: THE NUMBERS
Methotrexate and Me
It took the best part of a month, one more methotrexate injection, and yet another scan, for the tube to finally clear. During that time, I had blood tests every two days to make sure the HCG levels were dropping – and I got more and more anxious as time went on. Most of the ectopic pregnancy stories I’ve read make much of the injections, but I have to be honest: I was in such a state of anxiety at that point – and so desperate to avoid surgery – that they barely even registered with me. I remember having to have the injection in my butt, and it being not particularly dignified, but the nurses were so kind to me, and I was so far beyond caring that that was the absolute least of my worries.
I was sent home with a list of possible side effects from the injection, but I was very lucky and didn’t have any of them, so I really just had the anxiety to contend with. The anxiety, however, was absolutely off the charts. Every time we drove to Edinburgh to have blood taken, I’d be almost sick with nerves. The wait for the phone call with my results, meanwhile, was absolute agony – to the point that just the sound of Terry’s ringtone would send me into a complete panic.
During my month long wait, I continued to be so scared that the tube would rupture, or that the methotrexate wouldn’t work, and I’d have to have surgery anyway, that I had to continue taking Valium, and was basically unable to function normally. I spent most of the time in bed (On the plus side, I DID have time to re-read the entire Harry Potter series, so hey! Silver linings and all…), worrying that my ectopic pregnancy story was just NEVER going to end, basically, and… well, I wasn’t very easy to be around, let’s put it that way.
The HCG levels, meanwhile, rose to over 500 at their peak, and, at one point seemed to level out – at which point I had another (horrifically stressful) scan, and a second dose of methotrexate. The wait felt endless. At times, I honestly worried that my sanity was going to break because of the prolonged stress, which didn’t get any easier to deal with, even when the levels started to drop.
By Christmas day, my HCG had dropped to just 28 – to everyone around me, it seemed obvious that the nightmare was almost over, but, for me, my anxiety had never been worse. I knew it made no sense, but I was still absolutely TERRIFIED that the process was just NEVER going to end, and I got more and more scared with every blood test.
It wasn’t the best Christmas ever, tbh.
Finally, on New Year’s Eve 2016, I got the news I’d spent the whole month waiting for: my HCG levels were finally at zero, and the ordeal was over. I was relieved, obviously, but it was relief tinged with sadness. Yes, I was OK… but the reason I was OK was because another pregnancy had ended. What’s more, if we decided to try again, I now had an increased chance of having another ectopic – which I knew I wouldn’t be able to cope with.
It had been the worst month – and the worst experience – of my life, and it’s something I don’t think I’ll ever really “get over” exactly. And now we were left with the difficult decision of whether or not to try again…
Thanks for reading: and if you have your own ectopic pregnancy story to share, I’d love to hear from you












Rebecca
11/29/2016I’m so sorry to hear this, Amber– sending my thoughts and prayers for quick healing and peace!
The Other Emma
11/29/2016Wishing you a speedy recovery.
Joanna Glogaza
11/29/2016Sending tons of good energy <3
Charmaine Ng
11/29/2016Thank you for sharing your story. I really do hope you find peace soon. 🙂
– Charmaine
http://charmainenyw.com
Elise Hannah
11/29/2016Of course your health, both mental and physical , comes first. It’s trite and easier to say than do, but rest and recover. You will get through this with support from family and friends, and care from the NHS. X
Karen
11/29/2016Sending best wishes for a speedy recovery (as speedy as it can be, anyway) from Boston, MA. And even though you’re not religious, you’all be in my prayers for your well-being, but also that all your readers treat you with kindness as you go through this experience.
Sian
11/29/2016I’m so sorry to hear this, Amber, and I hope you’re feeling much better physically and mentally soon. I also suffer from health anxiety and have actually just returned from a panicked doctor’s appointment (I hate going too, but with working in an office, I need an actual diagnosis unfortunately!) for a repetitive strain injury in my wrist that I was convinced would result in surgery, so I understand to some extent your fears in the earlier part of your post. I hope the mammoth blog post helped you – it actually helped me realise there are others that suffer with similar fears to me – and I know that writing my thoughts out, whether on the internet or elsewhere, really helps me to sort through things in my head a bit. I know there isn’t a lot that can be said to help you in this situation but just know that we’re all wishing you the best and a speedy recovery!
Amber
11/29/2016Thanks, Sian: I’m very aware that most people won’t make it through this post, but I know a couple of other people who have very bad anxiety, and it’s always helped me to be able to talk to them and know I’m not the only one dealing with it, which is why I wanted to write this. Hope everything goes well with your wrist ?
Zoe
11/29/2016I am so very sorry for your loss x
Jennifer
11/29/2016Amber, I am so sorry you are having to deal with this now. I hope things go as smoothly as can be expected and that you make a good recovery. Anxiety is a miserable thing. Two people very close to me deal with severe anxiety so I have a slight understanding of what you are going through. It can be so hard when people only see the “unreasonable” reaction and don’t see how real that “unreasonable” reaction is. I will be thinking of you and I hope writing continues to be of help.
Wendy
11/29/2016What an absolutely shitty thing to happen and to have to deal with. I really hope the chemo does the trick as fast as possible. Just do whatever you need to do to feel better and stuff any nay sayers – I’ll happily give them a good verbal kicking for you if you like.
Now take the very best care of yourself and if there is anything I can do just let me know xx
Laura
11/29/2016Shit, I have nothing eloquent to say to this, but I wish for the very best! I hope you will have a quick and total recovery without the need for surgery and that there won’t be any long-term consequences. I am sending my best wishes and happiest thoughts your way – please get well soon!
Laura
11/29/2016I’m so sorry to read this – I will be thinking of you, hope everything goes well for you! x
Eva
11/29/2016Hi, Amber! Just wanted to say that I understand your anxiety completely (social anxiety in my case) and I’m glad that this was discovered as early as it was! I wish you all the strength and a fast recovery!
AH Jacqui
11/29/2016Oh Amber. I am so sorry that you have been going through all of this 🙁
Although it makes me very sad, I did enjoy reading this. This is an issue I can totally relate to and I know so many others in the same boat, I also thought your analogies at the beginning were totally on point!
I am so glad that you are recovering from this particular ordeal, and I’m sending healing hugs your way.
Anna International
11/29/2016Oh Amber! I am so sorry you are having to deal with this. I really hope the treatment all works as it should and the side effects are less than they have warned. You will get through this. As a fellow anxiety sufferer though, I know it might not seem like that right now. Sending hugs xx
Elizabeth
11/29/2016Oh, Amber. I really shouldn’t have read all this as I have my own anxiety but I really wanted to know how you were and what you were going through. It’s actually a relief to know you’ve caught it early so I’m sending lots of positive vibes your way.
Please keep writing and sharing. Get it all out. And it really does help some of us to know we’re not alone with our own mental health problems.
Lots of love
x.x.x
Forever Amber
11/29/2016Thanks, Jacqui – I really didn’t expect anyone to make it all the way through it, but it means a lot to me that you did: thanks so much for the support
AH Jacqui
11/29/2016You did a fantastic job of telling your story, and if people want to
unfollow because it’s not all sugar coated, then you should let them! ❤️
Deanna
11/29/2016Amber you are one of my favorite bloggers especially because you share more than fashion with us! I am glad it helps you to write, and am so very sad that you are experiencing this health issue. My daughter suffers from anxiety and I’ve seen how it affects her – and you’re right, when people discount her anxiety it makes her feel ashamed and belittled. I hope you are surrounded by people who love you and support you, and that you come safely through this scare without needing the surgery!
CiCi Marie
11/29/2016Amber, I’m really sorry to hear all this and my heart goes out to you. I can’t think of much more to say other than I’m thinking of you and wishing you a very speedy treatment. And write all you want, it’s your blog and if it makes you feel better screw everyone who’s rude about it. They don’t have to read it. xxx
Porcelina
11/29/2016I am so sorry for your situation Amber. Sending lots of positive vibes from Wales, be kind to yourself xxx
Emily
11/29/2016Oh Amber, I am so sorry to hear about what you are going through. I am thinking of you lots, sending virtual hugs and keeping everything crossed for your speedy recovery.
Claire
11/29/2016Oh Amber my dear, I think this is one of the bravest things I’ve read. I”m sorry you’re going through an awful time right now but I’m glad in whatever way this is helping.
Personally, I’m not here for the fashion. It’s how I found the blog sure, but you are why I read.
Louise
11/29/2016What a dreadful situation. I suffer with anxiety too, and fully admire you for being so open and honest. I’m sending you and Terry my best wishes and wish you a speedy physical recovery x
Amy Caulkins
11/29/2016Amber, I’m sorry you’re going through this. I’m an ICU nurse (with my own share of health anxiety, though I’m getting better at my avoidance behaviors) and I can honestly say your anxiety quite possibly saved your life here. An excellent post.
Hollie
11/29/2016So sorry this is happening to you. What a nightmare!! Wishing you a full recovery and a path to healing for anxiety.
Jen
11/29/2016So sorry to read this my heart really does go out to you, can’t imagine how your feeling right now. Wishing you a speedy recovery and sending lots of love and positive vibes.
Jen xx
JoW
11/29/2016Just wanting to send you hugs and hope that the chemo works. Take what ever time out you need, do what ever you need to do, and we’ll be here ready for when ever you’re ready xx
Sarah
11/29/2016So sorry to hear this Amber, wishing you a speedy recovery xxx
Ginarella
11/29/2016Dear Amber,
so far I was a silent reader of your blog. However, today I feel that I need to post a comment. I wish you all the best and fast recovery.
Best regards,
Ginarella
Trona
11/29/2016oh Amber I really really hope everything works out for you, sending much love you and your family’s way. I have anxiety and used to have agoraphobia so I know how awful those thoughts, feelings and physical symptoms can be. Hang in there <3 xxxxx
lila athanaselis
11/29/2016Hope you are not in a lot of pain, hope the treatment works and you are back on your feet again in your own time, we are all here for you, love you Amber xxx
Amber
11/29/2016Thanks, Lila, I could not possibly get through it without you all ❤️
Bry Jaimea
11/29/2016Sending as many positive thoughts your way, and saying thank you for being so open and honest with your anxiety. It’s an issue so many of us battle/suffer from/deal with, and the more awareness we can raise, the more we can make people see that it is an issue even the most normal, stylish, fabulous people have, the more help and acceptance we can get.
http://shortcutecompact.com
A
11/29/2016I’ve been following your blog for about 4 years now and I’ve never commented – because I am happy to read your excellent content. I am really sorry to read this and I do think that you are doing exactly what you should: acknowledging the problems and solving them one at a time. I appreciated this long post, it was very well written, engaging and informative about several serious issues that affect a lot of people. And as other said, this is your space and your business so do what you wish with it! Get well at your own pace and all the best.
Becky
11/29/2016Mahoosive hugs Amber – you are being insanely strong and you continue to do whatever you need to do to get you through each day xxx
Erin
11/29/2016Amber, I wondered why you had been rather quiet. I am so sorry that you are going through all of this! Sending all my positive thoughts to you and Terry and hoping everything goes as easily as possible <3
Geo Bag
11/29/2016Get well sooner. We love you both.
Amber
11/29/2016Thanks, George – love to you all, too ❤️
Sheena
11/29/2016I’m never quite sure what to say in situations like these as it never comes out quite right, however I just wanted you to know that I’m thinking of you and sending positive thoughts. Hope everything goes as well as it can and that you’re back on your feet very soon.
Call me M
11/29/2016I’m so sorry to hear this Amber! Of course health always comes first. So take all the time you need. But if writing makes you feel better, then you should keep doing it. I always loved your blog for being an online diary of yours, but also because I enjoy your writing and your sense of style as well. So I have no problem with the content changing a bit. Feel free to write anything you like.
I really wish for everything to go perfectly, and for you to have great news very soon. I hope you have a fast recovery!
Kat
11/29/2016Prayers from Boston MA Amber! I’m so sorry to hear all that you are having to deal with!! I can not begin to imagine what type of stress you are currently under 🙁 But in a small bid to offer whatever help I might, as a serial researcher of online info myself (thanks for all the sleepless nights WebMD…), here is a site I have found a lot of helpful info from – of particular interest, in anxiety. Please feel free to totally ignore! But as someone who has experienced sudden, random and unexplained anxiety myself, I feel like a total a** not sharing what helped!
http://nutritionfacts.org/topics/anxiety/
Katie
11/29/2016Hi Amber,
This all sounds terribly frightening for you and terrible for your anxiety. I’m a doctor in the US that has been following your blog for years. I just wanted to let you know if you have any questions, I can try and answer them and also to try and reassure you that I believe the scariest part of this has passed. I know you still have to go back in to check your blood quite a few times and this of course is scary due to your anxiety, but know that you should be getting better from this point, this is just to make sure. It may be hard to think of it this way, but at this point going to the hospital for follow up should be reassuring because you are moving forward towards better health each time and the people working there are there to make sure you get physically better. I hope you start feeling calmer, less anxious and better soon.
Amber
11/29/2016Thanks, Katie, that is incredibly reassuring to hear: thank you so much for commenting ❤️
Bex M
11/29/2016Oh Amber what an awful week! I’m so sorry it’s been so bad for you and Terry. I will keep you both in my thoughts and stay strong! ❤️ Xxx
Hana
11/29/2016I’m 100% sure you are strong enough to overcome this! Best of luck and a quick recovery. Any post will be treasured, but just take the best care of yourself now!
Chiarina
11/29/2016I was getting tears in my eyes while reading. I am so sorry for you and hope you get better quickly, both physically and mentally. A big virtual hug.
Jean
11/29/2016Awww sweet pea. I’m so so sorry one of your worst fears came to pass…. I absolutely 100 percent know this sounds terrible to say…but maybe it will be like that kind of immersion therapy. I know that’s shitty to say. Not helpful at. all. I suffer from general anxiety disorder and you could not have described it better…with the roller coaster and the plane. I have never seen it said better. Thank you for this. Thank you for being honest and real (and fashionable, heh… I suspect the reason it’s “fashionable” to confess to is because so many people suffer from anxiety and because eventually, as in your case, you can’t be all upbeat on a blog when you’re in the throes of it. Best wishes. And make use of that Valium, man. Zoned out is fine….. I really really hope the doctor helps with the anxiety. I’m still casting around myself. peace to you from the middle of the United States.
Myra
11/29/2016I’m gobsmacked at your courage in the face of your fears. Although I know you are not a believer, I believe in the power of prayer, and will keep you and Terry in my prayers, and am sending Angelic healing to you both ????
Karen
11/29/2016Sorry to hear your news Amber, wishing you a speedy recovery, I suffer from anxiety too and it’s hard to control so I get where you are with this. Love your blog and your style of writing, it’s good to get things out and we’re all here for you. Take care and get well soon xx
Jaclyn
11/29/2016Hi Amber, I’m so sorry to hear you are going through all of this – both the physical condition and the mental anxiety that goes with it. I’ve experienced small bouts of anxiety in the past but I can’t even imagine what it must be like to live with it in the way you do. Being pregnant myself right now too, your post touched me in ways I can’t explain and I truly feel a huge amount of empathy for you having to deal with this and go through it at all. For fear of adding to your symptoms I won’t say more than that and promise no ‘I have a friend’ stories, I just wanted to comment and let you know that I’ll be thinking of you and Terry and hope all goes as smoothly as it can and you take the time you need to recover. Lastly, I too know how cathartic writing can be, and feel similar to you in that it’s one of the only things that helps me in a down period so please never apologise for pouring your heart out on your blog – as much as i love your fashion posts, your personal ones will always be my favourite and I hope you continue to get some therapy from sitting down to write about whatever feels right to do so. Lots of love and hugs, Jaclyn
Beth
11/29/2016Hi Amber, like a few others here, I’ve been following and loving every aspect of your blog for years, but never commented, but I just wanted to say that I hope you get better soon and that you are in my thoughts 🙂
Sharon
11/29/2016Your blog is so well written and honest that I feel I know you and Terry fairly well from your posts. I’m so sad to read about what’s happening to you. Wishing you well. Xx
Nicola
11/29/2016So sorry to hear this Amber, I found your site randomly after searching for something about midi skirts, and was hooked! I read it because I just love your writing style, your humour and your honesty, (whatever you’re talking about. )
So sorry you are going through this. Sending you lots of good healing energy and i hope things are feeling better soon x
Carly
11/29/2016Really sorry to hear what you are going through Amber. I’ve had an ectopic pregnancy myself 7 years ago – I had wonderful care in the NHS. Whilst no two experiences are the same, I can appreciate some of what you are going through. I also think it is ok to be worried and anxious, after all it is a normal response to a threat. So don’t be too hard on yourself. My happy ending is the wonderful 3 year old boy snuggling into my side. i wish you a very speedy recovery x
Heather
11/29/2016My bedside manner is the worst so I will just say I will NOT unfollow you, no matter what you write, or under what influence ? You have such a talent for it. And I’m thankful you were able to catch it so early.
Catherine, Not Dressed As Lamb
11/29/2016Oh Amber this I was not expecting… All I can say is that I’m thinking of you, and I’m sending you virtual hugs and kisses from down south to up north. Take good care of yourself, keep writing as and when you want to – or not at all – and about whatever you damn well choose. I can see how getting it down “on paper” can be cathartic for you.
I’m wishing all good things in every aspect to come your way, you deserve it ?
Catherine xxxx
P.S. I may just drop you a very, VERY quick email – I know how emails can take up all your time so I promise it will only take about 10 seconds to read and about 20 seconds to reply, no thinking required (if that’s okay?) ???
Nicola M
11/29/2016Wishing you all the best Amber!
PoppyD
11/29/2016I’m so sorry to read this Amber, I can’t imagine what you and Terry must be going through. I’ve no idea how you’ve written about it so eloquently but you’ll have helped countless people by doing so, even if that wasn’t your intention with the post. It sounds like you know exactly how to handle this one step at a time, even if that must feel unspeakably overwhelming at the moment. I’m glad to read you’re being well looked after and wish you all the best with your recovery, both psychically and emotionally. To echo all the commenters here we love your blog for YOU, so don’t stress about a lack of content for how ever long it takes….though I know that can be easier said than done when a blog is your livelihood! Xxxxxx
Steph
11/29/2016Well, for all your fears of the latter part of this post not making sense, as always it reads far more put together and eloquently that I could ever have managed! I bet it must have been hard for you to write, but I’m glad it’s proving helpful to you to do so and I hope it continues to help you make sense of things. We always say ‘talking’ is the best healer, but sometimes doing that face to face with a real live human is more frightening than the issue itself – I know I’ve always found writing my thoughts down more soothing than classic ‘talking’ therapies. Writing is just talking in another form, after all. Here is another positive for you – I think this post will actually help a lot of people. For the last 6 months I’ve been on the receiving end of a partner with severe depression and anxiety which has only recently been diagnosed and it’s taken me such a long time to get my head around his problems and understand how best to help and support him. The problem is that we are all so hard wired to believe that the way we think and process things is the “right” way, that for a ‘healthy’ person (and I use that term loosely, because honestly I’m not sure I know anyone with a clean bill of mental health, and we’re all so different anyway how on earth are we meant to know who the truly healthy ones are?? I genuinely think the vast majority of us are a crisis or two away from suffering similar difficulties – one person’s run of the mill incident is another person’s life-changing trauma and we can just never know when it might happen to us) it is almost impossible to understand what is going through another person’s mind and why they aren’t responding the way we think they should. Hearing someone talk about their experiences so openly like this is so valuable to those on the other side of the fence. So in summary, I am happy to read your thoughts and feelings any time, whatever they may be. I’m glad they help you, and they help me too, so thank you! Hope you are feeling better as soon as you can xxx
Amy
11/29/2016Amber I read every word. I have suffered from anxiety my whole life and can relate (not to the health anxiety – I can’t even imagine!!) I only recently began medication and am being open about it hoping it helps others. I am sending lots and lots of positive thoughts your way!!
Anna
11/29/2016Sorry you’re having such a tough time, thinking of you x
Holly
11/29/2016Write whatever and whenever you want. I’ve loved feeling like I have another friend in Scotland. If it helps any-know that at least one person is going to read everything and hope the ordeal ends soon.
Jess Palmer
11/29/2016Amber- I have been reading for about a year but in my normal immersive way have read all the way back in the archives in that time. I feel I know you, Terry and Rubin. I am so so sorry to hear you are going through this. As a doctor from a very different speciality I will just say I hope my colleagues in the ERI and Livingston are looking after you with all the compassion you could wish for and you recover smoothly and swiftly.
Maria
11/29/2016I think that the n.1 priority is you taking all the time you need to get better, don’t worry about the ones who might lament the lack of fashion, as I’m pretty sure they wouldn’t think of fashion in similar situations, so I dare them to say a thing about it. I know these are tough times and I’m really sorry for what you’re going through; I can sort of understand what anxiety entails, I suffer too from it and it’s not a walk in the park, but I hope that with the help of your family and friends you will get through it well cared for. Anyway, I’m wishing you a speedy recovery and I really hope you will get better soon! xxx Maria
Laurie
11/29/2016I’m firmly in the camp that this is your space to write what you want, no matter whatI expect when I visit. This is a big thing in your life and if writing about it is what you need, write away…
I’m sending you all the good vibes I can send and wishing you all the best. I’m so sorry to hear about what’s happening and I hope you get better soon. 🙂
Ingrid farquhar
11/29/2016Good luck with the treatment Amber. Thank you for your immense bravery
Monica
11/29/2016Oh Amber, my heart goes out to you, what a terrible thing to happen. ? I hope you are not in pain and wishing you a speedy recovery. I totally understand your fear of pregnancy as Ive been afraid of pregnancy my entire life as an adult. I stayed childfree for years because of it but in the end I realised I had to overcome my fear if I ever wanted a child of my own. In my late thirties I fell pregnant and was scared shitless. But much to my surprise everything went fine and I had my daughter three years ago. Hang in there Amber and fingers crossed it will all be over very soon. ❤️?
Stephanie
11/29/2016I hardly ever comment, and I wish I had profound words.but I wanted to say that YOU, as a person, are more important than your blog and I don’t even know you personally. I follow your blog partly for the fashion, but partly because of the small parts of real person mixed in, not just fashion stories. So you do what you need to do.
Diane
11/29/2016Oh, Amber, I’m so sorry to read this (but am never sorry that you write about what’s going on with you). I could feel your anxiety and really related. I’m so glad you have Terry and your family and friends (and Valium) and I hope the treatment goes as smoothly as possible and you can get help with the anxiety after that. Love to you. xo
Marilyn
11/29/2016Dear Amber, Thinking of you all and wishing you a very speedy recovery indeed. You are stronger than you think you are. xx
Cindy Robb
11/29/2016A brave & eloquent post – I’m sure it’s helped a lot of folks who suffer similar problems. Sending warmest wishes – take care !
Annabelle
11/29/2016I’m very sorry for you and send you all my wishes of quick recovery, and hopefully without surgery. Moreover you did a great thing in writing such a long and detailed post about health anxiety: I didn’t know how awful it could be and only had such a thing (and, by reading you, a very light version compared to yours) once or twice in my life.
Just imagining you go through this so often makes me very empathetic. More people need to know. It’s very brave, especially in this situation to share this. Take care of you, Amber.
lalie
11/29/2016This too shall pass Amber. Be strong, as dark and miserable as things are, things will get better. It really won’t be that sad forever. I hope the test results are the one you hope for, the waiting time is torture. I am truly sorry you have to go through this, it’s so sad for both of you, and bloody unfair. You have to focus on the medical aspect for now, but then don’t be guilty to take all the time you need to grieve. It’s difficult, but you will be back to your happy self. I hope valium helps for now. I wish I knew what to write to help you, we haven’t met but you feel like a friend thanks to your blog.
Take care, thinking of you both
Lalie xxx
Alicja
11/29/2016Amber, my heart is with you now.
You’re very brave. Take care, my dear.
Anna
11/29/2016Oh Amber I am sorry you are going through all this and I am crossing everything for the outcome you wish for. I have generalised anxiety and social anxiety and I can agree with your description of the feeling. As somebody who is also currently undergoing chemotherapy I hope the side effects aren’t too nasty for you.
Amber
11/29/2016I’m so sorry to hear that, Anna: best of luck to you, too ?
Lia
11/29/2016I am so sorry to read you are going through this. I think you are incredibly brave telling your story. I hope that knowing your readers are sending you all our support helps you get through it.xxxxx
Mandy
11/29/2016Wishing the speediest and best possible outcome for you xxx
Tracey
11/29/2016Wishing you all the best for a speedy recovery Amber. Also sending hugs to Terry for being your rock!
Izabel
11/30/2016I have been in A&E witless with fear because SOMETHING was about to kill me dozens of times over the years . It’s a rotten thing to live with. I hope with all my heart the physical problem resolves as quickly and as easily as it possibly can and that, as hideous as this is, it might be the beginning of getting help with the psychological. Much love, Izabel.
Kat
11/30/2016I’m in the middle of the longest panic attack of my life and your entry has made me absolutely sob with relief. Not because something this awful is happening to you – but because what you wrote has touched me to the core in a way I haven’t been touched in a long time.
I’ve suffered with depression and anxiety my entire life. I nearly had a nervous breakdown and dropped out of school in my final semester. With the help of the most incredible teacher I’ve ever had, I made it. Then, a few months later I started grad school – as each month went by, everything worsened. I somehow made it to my second year before I dropped out of it. I felt like it was my only option since I was failed two of my classes at that point – and was nowhere near writing the required thesis. I have never been suicidal – but I have had dark days where I hid and sobbed in a corner or screamed or bit and hit my pillow to feel anything but this void I was in. My anxiety got so bad when I tried to work on an assignment for class, I had such a panic attack and would be thrown in a frenzy it might be days before I calmed down enough to work on it again. Then I sat down to work on it again and I was back in an anxiety attack. So I dropped out of school and began working at the first job I could find that I loathed and where I was emotionally abused for months.
Fast forward three years and I am worked hard to get to a state where I could go back and finish school. I’m on a probationary term and have two more weeks left which determine whether or not I can return. I’ve barely started on the essay due in 8 days. In two days, I also have a big medical exam – I’m in the process of applying for a fiance visa to the US and in order to get that visa, I have to go through a full medical checkup and then an interview with my partner. We also have to plan a mini-wedding to take place within 30 days of this interview. The planning has been a nightmare. We rarely fight and we’re really fighting over all of this. I had to take a two-week leave of absence to focus on school in order to get through this one thing and that’s terrifying me because I also really need the money.
And everything has suddenly really hit me to the point where I’ve been having an anxiety attack non-stop for over a week. I missed my class last week and had to leave work early. I’m breaking down and crying all the time. And above all I feel like I can’t breathe and knowing that it’s all in my head isn’t making it go away – but making it worse.
On top of all of this, I am not insured and cannot afford a counselor – I’d be on a year-long waiting for a psychiatrist too and it doesn’t even matter now with the possibility of me moving to another country happening.
Reading your struggles did not make me feel better about my troubles or distract me. I’ve always felt connected to you because of your writing – I know that sounds creepy and stalkery, but I’ve loved getting this little window into your life and have enjoyed getting to know the parts you’ve shared about yourself. So reading all of this gave me this immense feeling of relief and then more anxiety that this was happening to you, and that you’re going to be going through hell for the next while because of your hypochondria.
I’m sorry for how weird this is. Reading your entry made me want to spill all this out to you and I can’t bring myself to leave the page or delete this and leave a comment telling you how brave you are and how I’m rooting for you.
I do think you are incredibly brave and I’m so glad you have a wonderful support system behind you as you go through this. I hope that it’s all over soon.
Violeta, your Shoegal Out In The World
11/30/2016I am so sorry Amber to hear about you going something like this. I truly hope everything is resolved without any surgery and you take your time to recover both physically & mentally. I wish you all the best from Athens, Greece!
Violeta
Leigh Russell
11/30/2016Oh honey, I’m so sorry that all of this is happening to you and Terry right now. Sending positive healing vibes your way (you know I don’t do prayers) hope that you treatment is as quick and non invasive as possible. I’m so touched by your honesty and strength to be able to share such a difficult story with everyone. Please take comfort in the fact that telling all of these difficult truths will almost certainly help others, whether in understanding themselves or others…… That’s never a bad thing. Huge love. L x
Marty Drury
11/30/2016Earlier this year I spent two weeks not sleeping and running around my flat in a panic every night because of a strong, unexpected relapse of what is basically PTSD. Mild but still PTSD.
Over the years I’ve been on Valium, citalopram and now Prozac which does nothing for my moods but does mean I can’t panic like I used to.
I’ve had counselling at my GP practice twice (2 sets of six sessions each time with a three year gap between them) and I could run certificate courses in worrying and anxiety if I ever needed any extra cash. Though I’d worry two weeks beforehand about the venue hire and how much to charge.
At 35 years old, a lot of my life so far is filed under the heading: “crazy random stuff that mostly happened because I got anxious about things.”
I got therapy and I trained to be a psychotherapist and I’ve worked with a lot of people who have anxiety issues.
I still have my anxiety issues I work on. Right now, I’m worried that you’ll be thinking “who is this guy?” or “what the heck is he on about?” Or “why is he telling me all this?”
I wanted to qualify what I was saying with evidence I knew what I was talking about but now I’ve got this worry you’re gonna think I’m some random internet weirdo.
I’m also worried you’ll think I’m being disrespectful instead of being funny about my own anxiety (how I deal with my issues) which I am being. Or trying to be funny anyway.
I think we have a mutual friend somewhere along the lines and I read your blog. I probably could have just started with that as an into, couldn’t I? Anxiety makes me go off on massive tangents. You might have noticed that 🙂
Hopefully I’ve convinced you I can relate to the anxiety part of what you wrote about. Thank you for being so brave and open about what you’re going through as it encourages others to get help and support and breaks down mental health stigma.
I can’t imagine how hard it must have been to write that but I’m glad writing about it helps.
I’m so very sad at the awful things you’re going through and wish you all the best and hope things turn out okay.
Forever Amber
11/30/2016Thank you Marty, and please be reassured that I don’t think any of the things you’re worried about (although I totally get where you’re coming from as that’s how my head works, too!): quite the opposite in fact! The responses I’ve had to this post have helped me more than anyone will ever know, and I can’t thank you (and everyone else who’s been in touch) for writing them. I do intend to write more on this subject, because I really do believe that it’s something that should be spoken about, so thanks again for your kind words ?
Sara
11/30/2016I’m so sorry to hear about what you’ve been going through 🙁 I am not a regular commenter but I just wanted to say that I wish you well, and I hope you have a safe and speedy recovery. xo
Moira
11/30/2016Ache Amber, so sorry to hear that you’ve been having such a tough time. Thinking about you, Terry and your mum and dad xx
Ursula
11/30/2016I don’t have much to add to what everyone else has said – just wanted to say that I am very sorry about what has been happening to you, and that I am thinking of you and wish you a fast recovery. Get well soon!
Miss Kitty
11/30/2016I never know what to say in times like this, but I just had to let you know that I am thinking of you, hoping you get better soon, promise to read anything you choose to put on your blog (fashion or otherwise) and certainly will not unfollow you for it! *Hugs*
Helen Amelia
11/30/2016Wishing you the very, very best and may you soon feel tip-top!
Kirsty
11/30/2016I’m so sorry to hear this Amber – I can’t even begin to imagine what this is like for you. Wishing you all the best for a speedy recovery!
Petticoat
11/30/2016Thanks for your post, Amber. One of my relatives suffer from health anxiety, and so far I had not been able to understand him. Now I can better. Bless your courage! I know nothing I’ll say will help, so I just send you my most warm wishes.
Elaine
11/30/2016So sorry to read this Amber. I am a regular reader who always enjoys your writing both on style and on other subjects. I would like to join everyone in wishing you a very speedy recovery.
Best wishes
Elaine x
Melanie
11/30/2016So very sorry Amber. My thought are with you and Terry at this difficult time.
Emma
11/30/2016Oh Amber! I’m so very sorry. I’ve followed your websites for many years now and have always enjoyed your content and admired your writing, whether it’s fashion related or not! You’re being incredibly brave and will get through this. Thank you for sharing your story – judging by the comments, it’s helping so many people already. Wishing you all the best for your recovery and thinking of you at this difficult time xxx
Natasha
11/30/2016Dear Amber,
How are you doing? I have been reading your blogs for probably around 10 years now, and I never knew you were going through the same thing as I do, every single day of my life. When I saw your post yesterday, I started reading and left after a few sentences because of the dread that instantly gripped my belly. It took me several tries and the whole day to read the whole thing, during which time I even unfollowed you once because I couldn’t bear the thought of reading you were sick and then obsessing about it for days. I was crying through most of your post, because I understood every single word only too perfectly. I too have severe health anxiety, the kind that makes going to the doctor even for a cold almost unbearable. I have been trying to get help, but it’s a tough road. No one really understands what it’s like, and I don’t know if that’s a curse or a blessing – I feel deep shame at the thought of anyone comprehending the true extent of my problem. Thank you for being brave enough to write this post. I feel at least a tiny fraction less alone in all this. I hope you get better soon in every way. Thinking of you and sending you hugs.
Amber
11/30/2016Oh Natasha, I’m so sorry you have to deal with this too, and I’m incredibly touched that you read the post anyway. I promise to always put trigger warnings on these posts, and I will understand completely if you need to unfollow. I’m doing OK right now, and getting a lot of support from my family me friends, so thanks for your message, and please take care of yourself ?
dubliner in deutschland
11/30/2016I hope you are doing much better now and wishing you lots of strength over the next few days. I am also a little bit of a hypochondriac at times so I could relate to some of what you shared. There is a lot of cancer in my family and I regularly seem to have phases where I convince myself I have it in some form! I also hate reading articles about things like the hidden symptoms of ovarian or bowel cancer or whatever because there are always really vague symptoms such as “tiredness” or “stomach cramps” which of course I have on and off. And I also hate reading stories about a person who caught some crazy illness as even though it’s really unlikely I will also worry that such a thing could happen to me. And I also have a fear of doctor’s not taking me seriously. Luckily I am generally able to calm myself down, and so it is generally managable, and not as bad at all as what you describe. But I just wanted to share that I can relate to some of your worries. I hope that your therapist will be able to help you. And then I read about your ectopic pregnancy and what’s been going on the last few days. You poor thing!! Anyone would have found that scary. And I can imagine that such a thing that is generally really unlikely happening to you won’t help your health anxiety at all! (Is is the kind of thing that can run in families?) I think you are absolutely right to share what’s been going on here. Personally I don’t follow your blog just for the fashion. Sending you a lots of hugs.
Amber
11/30/2016No, it doesn’t run in families, we’ve just been incredibly unlucky, unfortunately. Since writing this, I’ve actually had quite a few people contact me to say they’ve also had ectopic pregnancies: it seems it’s more common than people realise, although still relatively rare, thankfully! When it happened to my mum, they didn’t have the benefit of early detection, or the option of using chemo for it (I think this particular treatment has only been used for around 20 years for ectopic pregnancy), so it was a very different situation: I’ve never been so thankful for modern medicine!
Theresa
11/30/2016I’m so sorry for your loss. You and Terry will be in my prayers.
L
11/30/2016I’ve “lurked” on your blog for a while now but have never commented before, although I enjoy reading your posts immensely. I’m so sorry you have to go through this, and I hope you are feeling better soon.
L
11/30/2016*I enjoy reading your usual posts – obviously I did not enjoy reading this one, although I do think you are very brave and commend you for speaking out about such things. It is so easy to feel alone, particularly when suffering mental health difficulties, and for many people with similar situations it can help immensely just to know there are other people out there who are brave enough to talk about it.
Deserae
11/30/2016Oh my. So sorry to hear you are dealing with so so much. I follow you for your humour and stories as much, or more than for fashion, so you’ve not lost a follower here. You are in effect, facing your worst fear. Not by choice, obviously, but you are showing an amazing amount of strength amidst really stressful circumstances. I really admire your ability to articulate what you are going through, and I wish you all the best for your recovery.
Annabel
11/30/2016I think the fact that this was posted yesterday and has over 90 comments sharing love and support show how much we, your readers, care about you. I don’t have health anxiety but I have my fair share of general anxiety and I can understand how you feel. It’s horrible but it will pass and you’re not alone. No matter how much you feel it, you’re not alone. There are others out there with health anxiety, other women that have gone through ectopic pregnancies and others that may not have gone through any of that and maybe don’t even understand what it’s like, but that care. Lean on others to help you go through this- it’s amazing how sharing your boulder with someone makes it that much lighter. And if writing about it for the next few weeks is what you need, then do so by all means. What’s important right now is your health and wellbeing
You have no idea how much I wish I could fly all the way to Scotland and hold you until everything is over. I obviously can’t, so I’m writing this comment because it’s the next best thing. I’m sending you tons of love all the way from Argentina and I promise to keep you on my thoughts. I’ll just go ahead and say something that always helps go thourgh a rough time: you will be alright. Maybe not in five minutes, maybe not in a day, maybe not in a week, but you will be. And while you heal, all of your readers will stand right behing you (metaphorically). Take care, Amber <3
Nicola Rollin
11/30/2016I know it must be weird to get well wishes from strangers (sorry!) but still needed to say that I’m rooting for you to get through the other side of this awfulness quickly and safely.
I’m also not religious and find it hard when people say things must have happened ‘for a reason’, or it’s fate or karma or some such. They often mean it from a good place, I’m sure, but it’s just not something I believe in either. So I won’t say anything like that.
I have been trying to think of something brilliant and inspirational to say since I read your news yesterday, but there isn’t anything that measures up.
So I will just say that I’m desperately hoping for you to get good news asap, so that you can try to put this behind you and find a bit of relief from all of the not knowing. Will miss your lovely posts terribly as I’m a selfish cow, but just get yourself well. Love to you, Terry and Rubin from a fellow shoe addicted introvert! xx
Sarah Rooftops
11/30/2016I’m so sorry. You ARE going to get through this and I have everything crossed that that will be quickly and smoothly. Big love. x
Vickie
11/30/2016I’m so sorry you’re going through this, and very grateful you wrote this post. I actually avoided it at first, because much as I love your writing and wanted to read it, my health anxiety is so bad that I knew whatever you had, I’d convince myself I had too. It was only when I saw your later post and that it was to do with pregnancy that I allowed myself to read it (as I am very definitely not pregnant right now, having just had a period!).
Your description of health anxiety is exactly my experience – so much so that I’m going to send this to my partner to read and hopefully understand a little better. Scared to move, ticking time bomb, being so anxious you can’t speak – yup, yup, yup. I’ve had a ton of CBT and did find it helpful for generalised anxiety disorder and rationalising the less severe awful thoughts that pop up, but it doesn’t really help when I have an actual symptom.
My thoughts are with you and I very much hope your body does what it needs to do and your recovery is quick.
Estelle Vale
11/30/2016A fantastic honest post that myself and I’m sure many others can relate too.
Liana
11/30/2016I am so sorry you have to go through this. I too sufer from health anxiety, not quite as bad as you described above but bad enough to make me avoid doctors at any cost. Or blood test, oh god I hate the waiting. And funny thing: I also cannot watch any movie that has a medical reference or shows someone having some serious health problems.
Anyway, here is how I try to cope with it, and what works for me – most times.
I have always been a little paranoid about my health but after I hit 30 (I am 36 now) I actually started having some health issues: some were minor, some were pretty big (by now I have had 3 biopsies, go me) and I needed 2 surgeries and lots and lots of medication. But at some point I was just exhausted of the panic/horror that accompanied every docto’s visit or blood test or interpreting my simptoms. So the first strep was to just stop googling. That helped a bit. First of all, it’s not reliable and second, I am not a doctor, I cannot see the big picture, even if I correctly identify a simptom, it doesn’t mean anything; all serious health problems are diagnosed after lots of tests and chek-ups not after one crazy night on webmd. Another thing was to just not think about it (actually, it was moslty pretending that nothing is happening, but somehow I managed to pull it off) and only deal with the doctor’s visit when I was in his office. The rest of the time I would ocupy my mind in any way I could: playing video games, reading, talking on the phone, watching movies, cooking or actually working (I am a software developer, that helps). But what helped the most was to realise that IT WILL PASS, I WILL GET THROUGH IT. If the simptoms do not get worse, it’s a good sign. If it was something I had experienced before, I was telling myself: “I have been here before and I know that I will not die from it”. Of course I still have anxiety, but this things help me cope with it. And it did get better. Maybe it sounds like flawed thinking to others but it helped me.
After all this will be over, you can look back and realise that this has been the worst thing that has happend to you healthwise and you made it through. That should be somehow empowering… That is how it works for me, at least.
I also have a somehow happy story about ectopic pregnancies: turns out I had one of those too, this spring. Caught really early, beggining of 5th week. By the end of that week I took the medicine and I was fine. There were no side effects, no pain, I don’t even remeber to have had a heavier period. You will be fine, too, I am sure!
I wish you all the best and hope that you will be able to not think about it, even if just for short periods of time, to give yourself some breaks.
Liana, from Transylvania (yes, vapires do exist ?)
Liana
11/30/2016*vampires
Lea Stewart
11/30/2016Amber am so sorry to hear about this though almost feel normal as I have had this since I was about 13 years old. Tried every tablet, counselling both group and individual, hypnotherapy and back to beta blockers now 160mg which has helped physical symptoms. Though the ones in my head the impending sense of doom something bad is going to happen or I have a serous disease or cancer are always there. Makes you pretty miserable huh! Meditating is my next attempt or self help in a hope can let myself properly enjoy life. A brilliantly written piece from yourself. Lea xxxx
Kelly Glen
11/30/2016I am so very sorry for everything you and Terry are going through at the moment. Having suffered with many different mental health problems for over 20 years I know just how debilitating these illnesses are. You have been very brave to write this very honest post. It must have taken a lot of courage for you to put your true feelings into words for other people to see. I hope that is helps you to see all the comments sending all their love to you and Terry. I hope that everything goes ok for you and that you will feel better soon. Make sure you take as much time off to rest as you need to and we will all still be here to show our support when you feel able to post again no matter what it is about.
Take care and all the best.
Viridiana
12/01/2016I’m so sorry you’re going through all this. It will get better, stay strong.
Ghalia
12/01/2016Thank you so much for sharing this with us, dearest Amber. Going through the comments, I feel like so many people have said exactly what I would like to. So, as another one of your loyal readers (who reads every last word you write, because your writing-style really is very engaging), I wish you a swift recovery as possible. It is wonderful to know that you have the support of so many loved ones in your life. It makes all the difference x
Ghalia
12/01/2016Thank you so much for sharing this with us, dearest Amber. Going through the comments, I feel like so many people have said exactly what I would like to. So, as another one of your loyal readers (who reads every last word you write, because your writing-style really is very engaging), I wish you a swift recovery as possible. It is wonderful to know that you have the support of so many loved ones in your life. It makes all the difference x
Louisa
12/01/2016What a brave piece, thank you for sharing though it must have been really hard. Sending best wishes with your treatment and also your general health, like others I love your blog not only for your fashion/beauty but for your blogs about yourself and your life.
Delaney
12/01/2016You’re a brave person, and I hope that writing here makes this journey a little bit easier. I’ll always read it! Thinking of you and your family.
Moni
12/01/2016Oh Amber, I’m so sorry to hear that!
Please feel hugged (very carefully!), and my thoughts and best wishes are with you and your family!
Sae
12/02/2016Thank you for having the courage to share this! I am an introvert with intense social anxiety as well, and as a fellow writer, your comment about words helping to make sense of my thoughts made a lot of sense. I also think it was nice that you tried to end the post with some positive things in your life–a good support system is one of the best things a person can have. Take care of yourself, and best wishes to you. <3
Nicky De Decker
12/02/2016Thank you for being so open about your anxiety. I also suffer from anxiety, although I haven’t been diagnosed with it (yet). I have been following your blog for 2 years or something now and I have never commented even though I wanted to, because I also have a bit of social anxiety. I love that you’re not “ashamed” to talk freely about your mental health issues, about being an extreme introvert and about personal subjects. I actually only follow bloggers who also write honestly about their personal life. So, thank you. I really admire you for this. I’m sure a lot of people who relate to you and what you’re going through have read your entire post and wouldn’t mind reading more about you, not just about dresses and make-up. It sucks that there is nothing anyone can say to lessen the anxiety. But I’m sorry for your loss and for what you’re going through Right now and I wish you a speedy recovery and hope you can get comfort from the ones who support you.
Sarah B
12/02/2016Another longtime reader here. Amber, I just wanted to express how deeply sorry I am for all that you’ve been going through. Sometimes blogs only provide just a small glimpse into others’ lives, but you are always so honest and I truly appreciate you letting us know what you are dealing with right now, even while at the same time I am so sorry to hear about the struggles you’ve faced. Despite the situation, your writing is just as eloquent as always, and I’m glad to hear that writing about it has helped you. I can relate a bit to that feeling as, although I rarely write (and have no talent for it…!), recently while going through a very stressful end to a relationship, I found it so cathartic to blast whatever I was feeling onto paper!!! I counted each day that I made it through as a triumph, counting one day at a time at first, until gradually I wasn’t even counting them anymore, and all was well. Each day you get through is a testament to your strength!
No matter the topic, your writing is always so full of spark, personality, truth, and honesty, and perhaps that is why so many of us readers feel that we have really come to know and love you through your words. At the very least, I am so glad that you were able to catch things early and begin the process to getting better as soon as you could. I echo the others here in sending my utmost best wishes for your recovery! Also, I would like to say as others have that it is YOU that we are here for, and that you should take all the time you need, and do whatever writing you need, to get through this. Take care! ~S
Bonita Vear
12/02/2016I’m so sorry to hear of your trying times Amber, wishing you all the best for healing and peace. Take care lovely, you will pull through this. xx bonita
Nicola Haliday
12/02/2016Dear Amber, I’m been reading your blog since just after your wedding post (the first photo I remember seeing was of the glorious buttons) and almost 10 years later I’m still reading because you are awesome, amusing, and quirky – you come across as so incredibly human that it’s endearing and this post really highlights that – it may not be as polished as usual but it is still a well told snippet of life. As a reader my stomach flipped reading it, I really hope things resolve for you in the quickest, smoothest, least invasive way possible!!
What Lou Wore 365
12/02/2016Christ Amber, I’m so sorry to read this, all of it. Wishing you a speedy recovery re: the ECP and much love in general to you and Terry x
Louise
12/02/2016Hi Amber. Hope you are better soon. I’ve had an ectopic pregnancy too. I’m sure your current treatment will work, but hoped it may reassure you to say that although mine was discovered too late to do anything but surgery, and I have general anxiety so was very scared – it was fine. All the medical staff were amazing as they knew how scared I was and they really looked after me. I was discharged from hospital the next day and recovered at home. I found the ectopic pregnancy trust a really useful source of information while I recovered too, I would recommend their site. Thinking of you.
Janine
12/03/2016So sorry to hear you’re having to go through this Amber. You just do what you need to do to get yourself through this and try keep your mind occupied with positive relaxing things. I suffer with anxiety and other issues (I just started to write them then realised that is NOT what you need to be reading, sorry xx). I’m hoping things get better for you soon and the medication alone works. Xx
Sophikita
12/05/2016Best wishes for a speedy recovery, sending virtual hugs (should you want them) and happy healing thoughts from this corner of the internet xx
Francesca
12/05/2016I am a fellow health anxiety sufferer. I am deeply sorry this is happening to you. You are a worthy human being and a good writer. I have followed your blog with pleasure for years now. I hope you recover happily and return to better days. Until then, take however much time you need. Good luck.
Nicola
12/13/2016Dearest Amber, thank you for having the guts to share this with us. I wish you peace, light & love in your mind, heart, body & soul. xox
Victorine Sara
01/21/2017Dear Amber, first my sister now passed was called Amber and my Mum named her whilst reading the book in the 70’s called Forever Amber :). In suffering with Health Anxiety and Panic Myself it really is equally as hard to explain how it feels, you described it just as it is, I know my description to my family and friends is imagine you are being dangled from a bridge by the thread of your knickers (trying to make light a little) the feeling of OMG! Am I gonna die, could I die and hellllllp! its truly a terrifying feeling! So coming across your blog is refreshing! There is also a side of having Health Anxiety (Hyperchondria) I have researched so much of course for and since the internet has been invented I must have had googled every possible condition! But it has lead me to become a Therapist and have a love of herbal cures and health practices. Now my family and friends contact me like I’m the local Witch Doctor. So there is always that Silver Lining….you can help others…. x